Drug Catalog - Product Detail
METFORMIN HCL 1000MG TAB 500CT
| NDC | Mfr | Size | Str | Form |
|---|---|---|---|---|
| 67877-0563-05 | ASCEND LABORATORIES | 500 | 1000MG | TABLET |
PACKAGE FILES



Generic Name
METFORMIN HCL
Substance Name
METFORMIN HYDROCHLORIDE
Product Type
HUMAN PRESCRIPTION DRUG
Route
ORAL
Application Number
ANDA090564
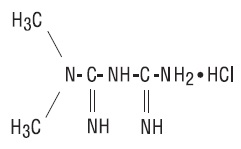
Description
DESCRIPTION Metformin Hydrochloride Tablets USP are oral antihyperglycemic drugs used in the management of type 2 diabetes. Metformin hydrochloride (N,N-dimethylimidodicarbonimidic diamide hydrochloride) is not chemically or pharmacologically related to any other classes of oral antihyperglycemic agents. The structural formula is as shown: Metformin hydrochloride is a white to off-white crystalline compound with a molecular formula of C 4 H 11 N 5 • HCl and a molecular weight of 165.63. Metformin hydrochloride is freely soluble in water and is practically insoluble in acetone, ether, and chloroform. The pKa of metformin is 12.4. The pH of a 1% aqueous solution of metformin hydrochloride is 6.68. Metformin Hydrochloride Tablets USP contain 500 mg, 850 mg, or 1000 mg of metformin hydrochloride. Each tablet contains the inactive ingredients povidone (K-30), povidone (K-90), pregelatinized starch,and magnesium stearate. In addition, the coating for the tablets contains artificial blackberry flavor, hypromellose and polyethylene glycol. Metformin Hydrochloride Structure
How Supplied
HOW SUPPLIED Metformin Hydrochloride Tablets, USP 500 mg - White to off-white, round, biconvex, film coated tablets debossed with G;10 on one side and plain on the other side. Bottles of 100 NDC 67877-561-01 Bottles of 500 NDC 67877-561-05 Bottles of 1000 NDC 67877-561-10 850 mg -White to off-white, round, biconvex, film coated tablets debossed with G;11 on one side and plain on the other side. Bottles of 100 NDC 67877-562-01 Bottles of 500 NDC 67877-562-05 Bottles of 1000 NDC 67877-562-10 1000 mg - White to off-white, oval, biconvex, scored, film coated tablets debossed with G and 12 on either side of the scoreline on one side and plain on the other side. Bottles of 100 NDC 67877-563-01 Bottles of 500 NDC 67877-563-05 Bottles of 1000 NDC 67877-563-10 Storage Store at 20°–25° C (68°–77° F); excursions permitted to 15°–30° C (59°–86° F). [See USP Controlled Room Temperature.] Dispense in tight, light-resistant containers with child-resistant closure. Manufactured by: Granules India Limited, Hyderabad-500081, INDIA MADE IN INDIA Distributed by: Ascend Laboratories, LLC Parsippany, NJ 07054 Toll Free No.: 1-877-272-7901 Nov 2016
Indications & Usage
INDICATIONS & USAGE Metformin Hydrochloride Tablets USP are indicated as an adjunct to diet and exercise to improve glycemic control in adults and children with type 2 diabetes mellitus.
Dosage and Administration
DOSAGE & ADMINISTRATION There is no fixed dosage regimen for the management of hyperglycemia in patients with type 2 diabetes with metformin hydrochloride or any other pharmacologic agent. Dosage of metformin hydrochloride must be individualized on the basis of both effectiveness and tolerance, while not exceeding the maximum recommended daily doses. The maximum recommended daily dose of metformin hydrochloride is 2550 mg in adults and 2000 mg in pediatric patients (10 to 16 years of age). Metformin hydrochloride should be given in divided doses with meals. Metformin hydrochloride should be started at a low dose, with gradual dose escalation, both to reduce gastrointestinal side effects and to permit identification of the minimum dose required for adequate glycemic control of the patient. During treatment initiation and dose titration (see Recommended Dosing Schedule ), fasting plasma glucose should be used to determine the therapeutic response to metformin hydrochloride and identify the minimum effective dose for the patient. Thereafter, glycosylated hemoglobin should be measured at intervals of approximately three months. The therapeutic goal should be to decrease both fasting plasma glucose and glycosylated hemoglobin levels to normal or near normal by using the lowest effective dose of metformin hydrochloride, either when used as monotherapy or in combination with sulfonylurea or insulin. Monitoring of blood glucose and glycosylated hemoglobin will also permit detection of primary failure, i.e., inadequate lowering of blood glucose at the maximum recommended dose of medication, and secondary failure, i.e., loss of an adequate blood glucose lowering response after an initial period of effectiveness. Short-term administration of metformin hydrochloride may be sufficient during periods of transient loss of control in patients usually well-controlled on diet alone. Recommended Dosing Schedule Adults – In general, clinically significant responses are not seen at doses below 1500 mg per day. However, a lower recommended starting dose and gradually increased dosage is advised to minimize gastrointestinal symptoms. The usual starting dose of metformin hydrochloride is 500 mg twice a day or 850 mg once a day, given with meals. Dosage increases should be made in increments of 500 mg weekly or 850 mg every 2 weeks, up to a total of 2000 mg per day, given in divided doses. Patients can also be titrated from 500 mg twice a day to 850 mg twice a day after 2 weeks. For those patients requiring additional glycemic control, metformin hydrochloride may be given to a maximum daily dose of 2550 mg per day. Doses above 2000 mg may be better tolerated given three times a day with meals. If higher doses of metformin are required, metformin hydrochloride should be used at total daily doses up to 2550 mg administered in divided daily doses, as described above. (See CLINICAL PHARMACOLOGY: Clinical Studies .) Pediatrics – The usual starting dose of metformin hydrochloride is 500 mg twice a day, given with meals. Dosage increases should be made in increments of 500 mg weekly up to a maximum of 2000 mg per day, given in divided doses. Transfer From Other Antidiabetic Therapy When transferring patients from standard oral hypoglycemic agents other than chlorpropamide to metformin hydrochloride, no transition period generally is necessary. When transferring patients from chlorpropamide, care should be exercised during the first two weeks because of the prolonged retention of chlorpropamide in the body, leading to overlapping drug effects and possible hypoglycemia. Concomitant Metformin Hydrochloride and Oral Sulfonylurea Therapy in Adult Patients If patients have not responded to four weeks of the maximum dose of metformin hydrochloride monotherapy, consideration should be given to gradual addition of an oral sulfonylurea while continuing metformin hydrochloride at the maximum dose, even if prior primary or secondary failure to a sulfonylurea has occurred. Clinical and pharmacokinetic drug-drug interaction data are currently available only for metformin plus glyburide (glibenclamide). With concomitant metformin hydrochloride and sulfonylurea therapy, the desired control of blood glucose may be obtained by adjusting the dose of each drug. In a clinical trial of patients with type 2 diabetes and prior failure on glyburide, patients started on metformin hydrochloride 500 mg and glyburide 20 mg were titrated to 1000/20 mg, 1500/20 mg, 2000/20 mg or 2500/20 mg of metformin hydrochloride and glyburide, respectively, to reach the goal of glycemic control as measured by FPG, HbA 1c and plasma glucose response (see CLINICAL PHARMACOLOGY: Clinical Studies ). However, attempts should be made to identify the minimum effective dose of each drug to achieve this goal. With concomitant metformin hydrochloride and sulfonylurea therapy, the risk of hypoglycemia associated with sulfonylurea therapy continues and may be increased. Appropriate precautions should be taken. (See Package Insert of the respective sulfonylurea.) If patients have not satisfactorily responded to one to three months of concomitant therapy with the maximum dose of metformin hydrochloride and the maximum dose of an oral sulfonylurea, consider therapeutic alternatives including switching to insulin with or without metformin hydrochloride. Concomitant Metformin Hydrochloride and Insulin Therapy in Adult Patients The current insulin dose should be continued upon initiation of metformin hydrochloride therapy. Metformin hydrochloride therapy should be initiated at 500 mg once daily in patients on insulin therapy. For patients not responding adequately, the dose of metformin hydrochloride should be increased by 500 mg after approximately 1 week and by 500 mg every week thereafter until adequate glycemic control is achieved. The maximum recommended daily dose is 2500 mg for metformin hydrochloride. It is recommended that the insulin dose be decreased by 10% to 25% when fasting plasma glucose concentrations decrease to less than 120 mg/dL in patients receiving concomitant insulin and metformin hydrochloride. Further adjustment should be individualized based on glucose-lowering response. Specific Patient Populations Metformin hydrochloride is not recommended for use in pregnancy. Metformin hydrochloride is not recommended in patients below the age of 10 years. The initial and maintenance dosing of metformin hydrochloride should be conservative in patients with advanced age, due to the potential for decreased renal function in this population. Any dosage adjustment should be based on a careful assessment of renal function. Generally, elderly, debilitated, and malnourished patients should not be titrated to the maximum dose of metformin hydrochloride. Monitoring of renal function is necessary to aid in prevention of lactic acidosis, particularly in the elderly. (See WARNINGS .)
